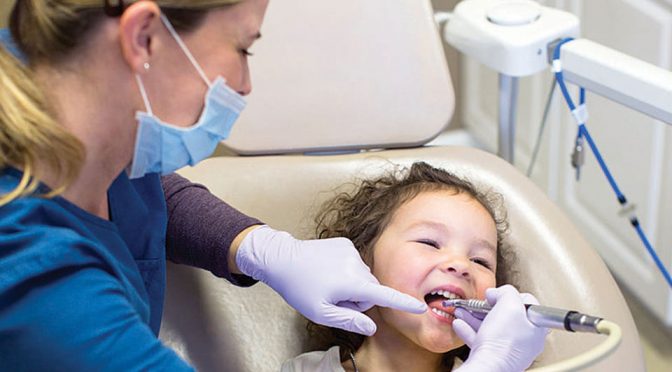
When Melanie Simmer-Beck, a UMKC School of Dentistry professor, began working to bring better oral health care to children in Kansas, she was often surprised at the level of tooth decay she and her colleagues saw in their young patients.
The children who came to in-school clinics in several Olathe, Kan., public schools often were sitting in a dental chair for the first time. Many times the state of their teeth was shocking. But surprisingly, the kids barely seemed to notice the pain they must have been feeling.
“They were so used to it, they thought it was normal,” she says.
In light of ongoing provider shortages — especially for low-income patients without resources to pay for care — some states, including Kansas, are trying to provide care to more patients by allowing dental hygienists to go into communities and provide preventive dental care without direct dentist oversight. More complicated cases are referred to dentists, but routine cleanings and care can be taken directly to the communities that need it most.
Simmer-Beck, a dental hygienist by training, has been on the leading edge of an effort to study the effectiveness of expanding the dental health workforce — allowing registered dental hygienists to deliver patient services without the direct supervision of a dentist.
Now, Simmer-Beck and Pat Kelly, a UMKC School of Nursing and Health Studies professor, are working together on a grant from the National Institutes of Health, specifically the National Institute for Dental and Craniofacial Research (NIDCR), to look further into the effectiveness of this practice.
“We’re just hoping we can do a good analysis and not have biased results. But in my heart of hearts I’m hoping to show that this legislation — expanding the dental health workforce — would make a difference,” Kelly says.
The five-year grant, worth up to $4.38 million, will compare dental models in Kansas, where dental hygienists are allowed direct patient access, to those in Missouri, where dental hygienists must provide dental care in the presence of a dentist.
“Our hypothesis is that the model in Kansas will provide as good, if not better, care as the traditional model, and that it will be more cost-effective,” Simmer-Beck says.
Children from certain racial and ethnic groups or from families with low levels of education and income are far more likely than other children to develop oral diseases, including tooth decay. Last year, the National Center for Health Statistics reported that Hispanic and Latino children and African-American children are about twice as likely as white children to have untreated tooth decay in primary teeth. One of the main reasons for the disparity is that there simply aren’t enough dentists to provide care.
Simmer-Beck’s Ph.D. educational program, supported by a NIDCR training grant (T32), centered around data collected through the public school clinics in Olathe, Kan., which the School of Dentistry organized and operated under a grant from the REACH Healthcare Foundation. Based on data collected at those clinics, Simmer-Beck found that getting children to the dentist more often, even if care was provided only by a dental hygienist, improved the oral health status of low-income children who would not otherwise have received care.
Simmer-Beck and Kelly hope the NIH study, done in collaboration with the Kansas Bureau of Oral Health School Sealant Program, will help add to the research that supports additional programs like the one in Kansas that allows hygienists to provide more care.
“This project will identify cost-effective, evidence-based strategies that improve access to dental providers in rural and urban underserved communities and ultimately reduce the number of children in Kansas who experience pain and suffering from oral health problems that are largely preventable,” Simmer-Beck says.
The NIH grant funding the study is part of 10 research cooperative agreements awarded nationally, aimed at eliminating inequities in access to care and improving the oral health of children. They support the Multidisciplinary and Collaborative Research Consortium to Reduce Oral Health Disparities in Children, a new initiative of NIDCR.